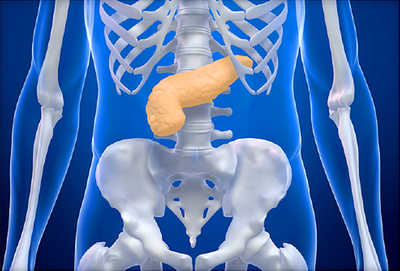
If you are asking what organ produces insulin, the answer is the pancreas. More specifically, insulin comes from beta cells inside pancreatic islets (small hormone-making cell clusters) in the pancreas. This matters because insulin helps move glucose, or blood sugar, from the bloodstream into cells for energy. Without enough usable insulin, blood glucose can rise and contribute to diabetes-related health problems.
Key Takeaways
- The pancreas makes insulin in beta cells.
- Those beta cells sit within pancreatic islets, also called islets of Langerhans.
- Insulin helps lower rising blood glucose after meals.
- Glucagon, another pancreas hormone, helps raise blood glucose when needed.
- Diabetes can involve low insulin production, insulin resistance, or both.
What Organ Produces Insulin?
The pancreas is both an organ and a gland, and it has more than one job. It sits deep in the upper abdomen, behind the stomach. Part of the pancreas releases digestive enzymes into the small intestine. Another part releases hormones directly into the bloodstream. Insulin comes from this hormone-making, or endocrine, part.
People also ask which gland secretes insulin because insulin is a hormone. In that sense, the pancreas acts as an endocrine gland. It secretes insulin, glucagon, and other signaling hormones that help the body keep blood glucose within a workable range.
The key insulin-making cells are beta cells. These cells are grouped inside pancreatic islets, also called islets of Langerhans. Alpha cells in the same islet system make glucagon. The result is one organ with a built-in balancing system: insulin helps move glucose out of the blood, while glucagon helps release stored glucose when levels fall.
Why it matters: Blood sugar control depends on both insulin supply and insulin response.
CanadianInsulin.com acts as a prescription referral platform, not a prescribing clinician.
How Beta Cells Make and Release Insulin
Beta cells release insulin when blood glucose rises, especially after carbohydrate-containing food. The process is not a simple on-off switch. Beta cells sense changing glucose levels, process insulin inside the cell, then release stored insulin into the blood when the body needs it.
Once insulin reaches the bloodstream, it attaches to insulin receptors on cells. These receptors work like signal receivers. When the signal is strong enough, many body cells can take in glucose and use it for energy. The liver and muscles can also store some glucose as glycogen, a reserve form of sugar.
This is the core insulin hormone function. It does not just reduce a number on a lab report. It supports energy use, storage, and metabolic stability. When insulin action is weak or insulin supply is too low, glucose can remain in the blood instead of entering cells efficiently.
The pancreas does not regulate blood sugar alone. The liver, muscles, fat tissue, digestive hormones, nervous system, and kidneys all contribute. Still, the pancreas is central because beta cells provide the insulin signal that many tissues need to handle glucose after meals.
Insulin, Glucagon, and the Pancreas’s Two Jobs
Insulin and glucagon are counterbalancing hormones made by the endocrine pancreas. They do not perform identical tasks. Insulin responds mainly to rising glucose. Glucagon becomes more important when the body needs to bring glucose back up, often between meals or during fasting.
| Pancreas output | Where it comes from | Main role | Plain-language effect |
|---|---|---|---|
| Insulin | Beta cells in pancreatic islets | Helps lower rising blood glucose | Supports glucose entry into cells and storage |
| Glucagon | Alpha cells in pancreatic islets | Helps raise low blood glucose | Signals the liver to release stored glucose |
| Digestive enzymes | Exocrine pancreas tissue | Help digest food in the small intestine | Break down fats, proteins, and carbohydrates |
This is why the pancreas can confuse readers. It is not only an insulin organ. It is also a digestive organ. The endocrine pancreas sends hormones into the blood. The exocrine pancreas sends digestive fluids through ducts into the gut.
When someone asks which gland secretes insulin and glucagon, the most accurate short answer is the endocrine part of the pancreas. When someone asks which organ regulates blood glucose levels, the pancreas is the main hormone source, but blood glucose regulation also depends on how the rest of the body responds to those signals.
Why Insulin Production Matters in Diabetes
Diabetes involves a mismatch between insulin supply, insulin action, or both. In type 1 diabetes, the immune system damages beta cells, so the pancreas makes little or no insulin. In type 2 diabetes, many body tissues respond less effectively to insulin. Beta cells may make extra insulin for a time, but they may not keep up with the body’s needs.
That difference matters because the underlying problem is not the same for every person. One person may have too little insulin production. Another may have insulin resistance, where cells do not respond well to insulin. Some people have both problems. Lab results, symptoms, medical history, and clinician assessment help sort this out.
If the pancreas stops producing enough insulin, glucose can build up in the bloodstream. Cells may struggle to use glucose well, even when blood glucose is high. In severe insulin deficiency, the body may break down fat for energy and produce ketones. A dangerous ketone buildup can become diabetic ketoacidosis, which needs urgent medical care.
On this site, the Diabetes Condition hub groups diabetes-related browsing options. The Diabetes Category is a browseable product-category list for diabetes-related items, not a substitute for clinical guidance.
Insulin can also be affected by rarer pancreas-related conditions. For example, an insulinoma is a tumor that can release insulin and contribute to low blood sugar episodes. For more background on that topic, see Insulinoma Causes.
Where needed, prescription details may be checked with the prescriber before referral steps continue.
Common Blood Sugar Misconceptions
Pancreas biology helps explain why food questions rarely have one universal answer. Blood glucose changes depend on the food, the person, timing, activity, medications, insulin sensitivity, and the starting glucose level. A food that raises glucose quickly in one setting may behave differently in another.
Low blood sugar needs speed
When a person with diabetes has a low blood sugar plan, it often prioritizes a fast-acting carbohydrate. Foods with fat and protein can digest more slowly. A peanut butter sandwich contains carbohydrate, but it also contains fat and protein, so it may not be the fastest option for an urgent low. A clinician-approved hypoglycemia plan is important for anyone at risk.
No single food is always worst
There is no single worst food for every person’s blood sugar. Sugary drinks and large portions of refined starch can raise glucose quickly for many people, but total pattern, portion size, and timing matter. Lab data and home glucose patterns often teach more than one isolated food rule.
Morning drinks still count
Water is generally a neutral morning choice for blood glucose. Sweetened coffee drinks, juice, regular soda, and some smoothies can add carbohydrates quickly. Caffeine may also affect some people differently. If you use insulin or glucose-lowering medication, morning drink choices should fit the plan your clinician gave you.
Quick tip: Keep a written low-blood-sugar plan if your clinician says you are at risk.
Practical Questions to Discuss With a Clinician
The most useful next step is to connect pancreas facts with your own health context. General anatomy explains where insulin comes from, but it does not diagnose diabetes, predict insulin needs, or replace individualized care.
- Blood glucose patterns: Ask how fasting and after-meal numbers differ.
- A1C meaning: Clarify what the result suggests over time.
- Symptoms: Report thirst, frequent urination, shakiness, sweating, or confusion.
- Medication fit: Review how each treatment relates to insulin supply or response.
- Low glucose plan: Know what to do if levels drop.
- Pancreas history: Mention pancreatitis, surgery, or endocrine conditions.
- Follow-up testing: Ask which labs or checks matter next.
Bring a current medication list and any home glucose records if you have them. Include nonprescription supplements, recent steroid use, and major diet or activity changes. These details can help a clinician interpret whether the issue is likely insulin production, insulin resistance, another hormone problem, or a mix of factors.
Dispensing, when permitted, is handled by licensed third-party pharmacies.
Human Biology and Pet Diabetes Need Different Context
Human and animal insulin biology overlap, but care decisions are species-specific. Dogs, cats, and people all rely on insulin signaling, yet diagnosis, monitoring, medication selection, and dosing decisions differ. A human diabetes article should not be used to manage a pet, and pet-focused material should not guide human treatment.
CanadianInsulin.com also provides pet-specific resources for readers caring for animals. For a broad starting point, see Pet Diabetes. For urgent cat-specific background, see Diabetic Ketoacidosis in Cats. Medication discussions differ by species, so veterinary-focused pages such as Vetsulin vs Novolin and Humalog for Dogs should be read in that context.
Pancreas-related conditions can also appear in veterinary care. For animal-specific background, see Insulinoma in Dogs and Pancreatitis in Cats. A veterinarian should guide diagnosis and treatment decisions for pets.
Authoritative Sources
These references support the anatomy and blood sugar concepts discussed above.
- For pancreas hormone basics, see the Endocrine Society overview of pancreas hormones.
- For diabetes definitions, see the NIDDK overview of diabetes.
- For low blood sugar safety context, see the American Diabetes Association hypoglycemia resource.
Further Reading and Recap
The pancreas makes insulin through beta cells in pancreatic islets. Insulin then helps the body move glucose from blood into cells and supports glucose storage. Glucagon works in the opposite direction when the body needs more glucose available in the blood.
Knowing this basic pancreas function can make diabetes terms easier to understand. It can also help you ask clearer questions about lab results, symptoms, insulin resistance, low blood sugar plans, and medication discussions.
This content is for informational purposes only and is not a substitute for professional medical advice.