Please note: a valid prescription is required for all prescription medication.
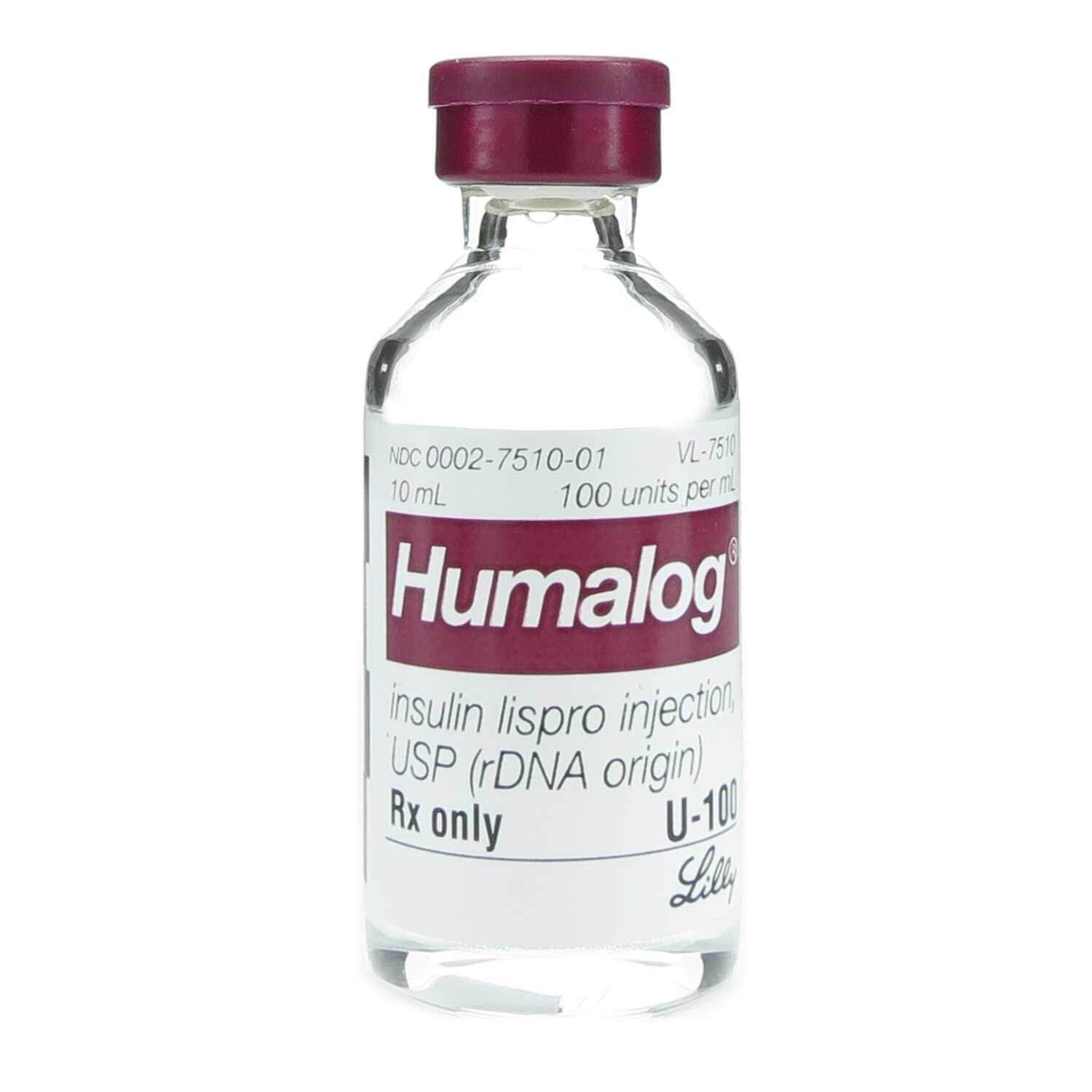
Looking at the Humalog Vial price before you order online? Compare the current listed pricing, the U-100 vial presentation, quantity options, and key safety basics before checkout. A valid prescription is required for a Humalog insulin vial order, and the selected product should match the form and strength written by your prescriber.
Humalog is insulin lispro, a rapid-acting insulin used around meals or correction dosing as directed. On this page, you can check the 100 units/mL vial details, understand what affects cost and access, and review storage needs for this temperature-sensitive medicine.
Humalog Vial Price and Available Options
The current listed price should be compared with the exact vial presentation in the product selector. For Humalog Vial 100 units/mL, the key details are concentration, vial volume, total units, and quantity selected. A lower-looking amount may not compare evenly if another listing contains a different total volume, device, or pack size.
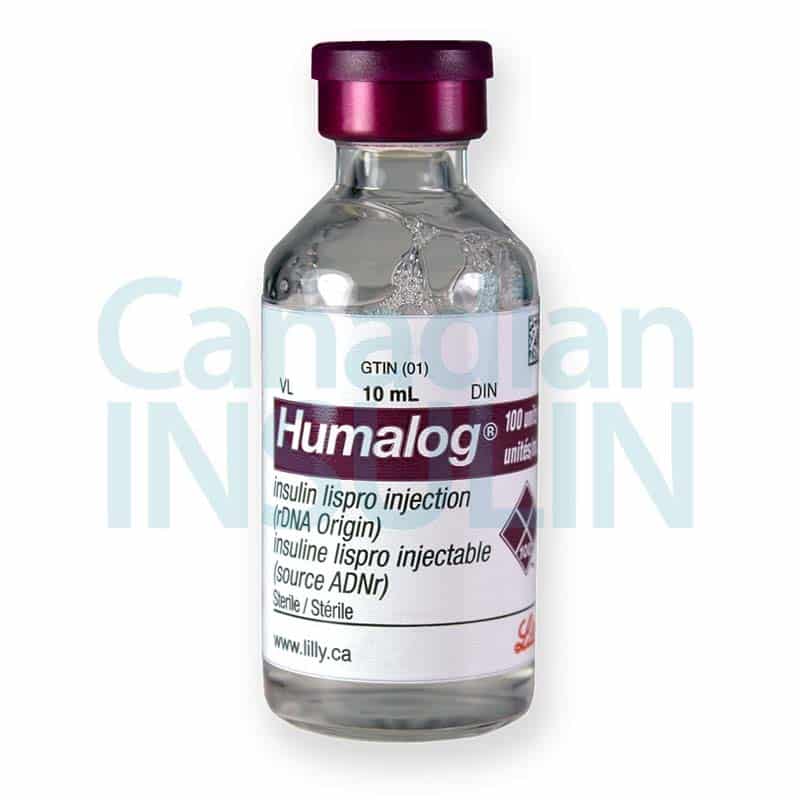
This listing is for a 10 mL U-100 vial. At 100 units/mL, a 10 mL vial contains 1,000 units in total. That total content is not a recommended dose; it is the amount of insulin in the container, which helps you compare the Humalog 10 mL vial price with other presentations.
- Strength: U-100, meaning 100 units of insulin per mL.
- Volume: 10 mL, which equals 1,000 units per vial.
- Form: Injectable solution supplied in a multiple-dose vial.
- Quantity: Match the selected number of vials to the written order.
- Presentation: Vials, pens, and cartridges are not interchangeable at checkout.
If you are comparing Humalog Vial without insurance, focus on the final listed product, quantity, and any handling charges shown before checkout. Coverage and retail pharmacy amounts can differ from Humalog Vial cash pay listings, so use the active page details rather than old web estimates.
When comparing prescribed mealtime insulin options, the Rapid Acting Insulin collection can help you check presentation types without mixing them into one vial-to-vial comparison.
How to Order Online
Choose the vial presentation that matches your prescription, then keep your prescriber information and current order details close during checkout. Prescription details may be reviewed or verified when needed, especially if the product, strength, or quantity does not clearly match the directions supplied.
Before placing the order, confirm that the product name, active ingredient, concentration, and vial size are correct. Humalog U-100 vial, Humalog KwikPen, Humalog cartridges, and premixed Humalog products are different items, even when they share part of the same brand name.
- Match the strength: Confirm U-100 and 100 units/mL.
- Check the form: Select vial only if that is what was prescribed.
- Review quantity: Make sure the number of vials fits the order.
- Prepare details: Keep prescriber and pharmacy information available.
- Check handling: Review temperature-sensitive shipping notes before checkout.
For US delivery from Canada, plan ahead because insulin is temperature sensitive and should not be treated as an emergency refill option. Checkout may show handling or supporting-document steps based on the selected item and destination.
Quick tip: Review any express, cold-chain shipping notes before placing the order, then plan refills before the vial runs low.
Vial Strength, Contents, and Product Details
Humalog insulin lispro vial is an injectable solution, not a pen, cartridge, or premixed insulin. The active ingredient is insulin lispro, a rapid-acting insulin analog. Analog means the insulin molecule has been modified to change how quickly it starts working after injection.
The insulin lispro 100 units/mL vial is commonly described as U-100. The concentration matters because syringes, pump reservoirs, and dosing instructions must be compatible with the prescribed insulin. Do not select a different concentration or device style unless your clinician changes the order.
| Product detail | What to check |
|---|---|
| Active ingredient | Insulin lispro |
| Concentration | 100 units/mL, also called U-100 |
| Vial volume | 10 mL per vial |
| Total contents | 1,000 units per 10 mL vial |
| Form | Injectable solution in a multiple-dose vial |
| Typical use route | Subcutaneous injection, or pump use only if prescribed and compatible |
The Humalog Vial 10 mL presentation may be selected by people who draw doses with an insulin syringe or use a compatible pump as prescribed. Pumps have model-specific requirements, so match the insulin and reservoir instructions supplied by the pump manufacturer and your clinician.
Device preference can also affect product selection. The Insulin Pen Vs Syringe resource compares practical device differences, but your chosen listing should still follow the current prescription.
What This Rapid-Acting Insulin Is Used For
Humalog is used to help improve blood glucose control in people with diabetes mellitus. It is a rapid-acting insulin, so it is often used as bolus insulin, meaning mealtime or correction insulin, within an overall diabetes plan.
Some people use rapid-acting insulin with a separate long-acting insulin. Others may use it in an insulin pump if their care plan and device instructions allow it. The vial does not determine your dose schedule; your clinician sets that based on glucose patterns, meals, activity, and other medicines.
Because insulin plans are individualized, the most useful product decision is to match the listing exactly. Check whether your written order names Humalog, insulin lispro, U-100, vial, 10 mL, or another presentation. Small wording differences can point to a different product.
Storage, Handling, and Travel Basics
Insulin is sensitive to temperature, freezing, heat, and light. Before first use, unopened Humalog vials are generally stored in a refrigerator, according to the product label. Do not freeze insulin, and do not use a vial that has been frozen.
After first use, a Humalog multiple dose vial may usually be kept refrigerated or at room temperature below the label limit for a limited in-use period. Many Humalog vial instructions reference discarding after 28 days in use. Always follow the carton, package insert, and pharmacist instructions for the product received.
Check the liquid before use. Humalog should be clear and colorless. Do not use it if it looks cloudy, thickened, colored, or contains particles. Also avoid using insulin after the expiration date or after the in-use discard date has passed.
- Refrigeration: Store unopened vials as directed on the label.
- Freezing: Discard insulin that has frozen.
- Heat exposure: Keep away from hot cars and direct sunlight.
- Travel: Carry insulin in temperature-aware packaging when needed.
- Inspection: Check appearance before each use.
The Insulin Storage Temperature resource outlines temperature basics that can help you prepare for home storage and travel planning.
Why it matters: Storage problems can make insulin less reliable, even when the vial looks acceptable.
Safety Information Before Buying
The most common serious risk with insulin lispro is hypoglycemia, or low blood sugar. Symptoms can include shakiness, sweating, fast heartbeat, hunger, confusion, weakness, blurred vision, or headache. Severe hypoglycemia can cause seizure, loss of consciousness, or death if not treated promptly.
Do not use Humalog during episodes of hypoglycemia. It is also contraindicated in people with a serious hypersensitivity to insulin lispro or any ingredient in the product. Allergic reactions may include rash, itching, swelling, wheezing, trouble breathing, very low blood pressure, or anaphylaxis.
Other possible adverse effects include injection-site reactions, lipodystrophy, which means changes in the fat tissue under the skin, itching, rash, weight gain, and edema, or swelling from fluid retention. Rotating injection sites within the recommended area can reduce repeated irritation, but site selection should follow clinician instructions.
Insulin can also contribute to hypokalemia, meaning low potassium, especially in higher-risk settings or when used with medicines that affect potassium levels. Signs such as muscle weakness, abnormal heartbeat, or severe fatigue need clinical attention.
- Low sugar risk: Know your treatment plan for hypoglycemia.
- Allergy symptoms: Seek urgent help for breathing trouble or swelling.
- Skin changes: Report lumps, thickening, or repeated irritation.
- Potassium concerns: Ask about monitoring if you are at risk.
- Product errors: Check labels carefully before every use.
Never change dose, timing, insulin type, or device based only on a product listing. If the vial received looks different from expected, pause and ask a pharmacist or clinician before using it.
Interactions and Monitoring Checks
Many medicines can change how insulin affects blood glucose. Some may increase the chance of hypoglycemia, while others may raise blood sugar and make control harder. Alcohol can also affect glucose patterns and may increase low blood sugar risk in some situations.
Medicines that may interact include other diabetes treatments, corticosteroids, diuretics, thyroid medicines, some antidepressants, beta-blockers, ACE inhibitors, angiotensin receptor blockers, and certain antipsychotics. Beta-blockers may also hide warning signs such as fast heartbeat, making glucose monitoring especially important.
Illness, changes in meals, activity changes, kidney or liver problems, pregnancy, and surgery can all affect insulin needs. These situations are reasons to speak with a clinician, not to self-adjust based on product availability or online information.
- Glucose monitoring: Follow the testing plan set by your clinician.
- Medicine changes: Report new prescriptions or supplements.
- Sick days: Use the care plan provided by your diabetes team.
- Pump concerns: Address unexplained highs quickly with clinical guidance.
Compare Related Presentations
Humalog products are not all supplied the same way. A vial may suit people who use syringes or certain pump systems. A pen may be preferred when portability and built-in dose dialing are part of the prescribed plan. A cartridge is a separate presentation for compatible delivery systems.
If your prescriber wrote for a pen, compare the product details for Humalog KwikPen rather than choosing a vial. If the order specifies cartridges, check Humalog Cartridge instead. These options should not be substituted without clinical direction.
| Presentation | Practical difference |
|---|---|
| Vial | Requires compatible syringes or an approved pump setup. |
| Pen | Uses a prefilled pen device with compatible pen needles. |
| Cartridge | Fits specific cartridge systems rather than a standard vial setup. |
| Premixed insulin | Contains different insulin components and is a separate treatment type. |
Other rapid-acting insulins, such as insulin aspart or insulin glulisine products, may appear in the same broader class. They have different product names, labels, and device options. Compare them only when your clinician has discussed switching or substitution.
Authoritative Sources
Manufacturer Pricing Information gives U.S. list-price context, but your out-of-pocket amount can differ from the amount shown on this product page.
For label-specific use, safety, storage, and discard instructions, follow the current package insert included with your insulin and the directions provided by your licensed healthcare professional.
This content is for informational purposes only and is not a substitute for professional medical advice.
{acf_product_technical_information}
Express Shipping - from $25.00
Shipping with this method takes 3-5 days
Prices:
- Dry-Packed Products $25.00
- Cold-Packed Products $35.00
Standard Shipping - $15.00
Shipping with this method takes 5-10 days
Prices:
- Dry-Packed Products $15.00
- Not available for Cold-Packed products
How many units are in a 10 mL vial?
A U-100 insulin lispro vial contains 100 units per mL. A 10 mL vial therefore contains 1,000 total units. That number describes the contents of the container, not a single dose or a recommended daily amount. Your clinician determines how many units to use based on your diabetes plan, meals, glucose readings, and other factors.
How should insulin lispro be stored?
Unopened vials are generally kept refrigerated according to the product label. Do not freeze insulin, and do not use a vial that has been frozen. Once in use, Humalog vials are usually kept refrigerated or at room temperature within the label limit for a defined period, often 28 days. Check the carton and package insert for the exact instructions supplied with your product.
What side effects need prompt medical attention?
Severe low blood sugar needs urgent attention, especially if it causes confusion, seizure, loss of consciousness, or inability to swallow safely. Also seek help for signs of a serious allergic reaction, such as swelling of the face or throat, trouble breathing, wheezing, widespread rash, or faintness. Symptoms of very low potassium, including severe weakness or abnormal heartbeat, should also be discussed urgently with a clinician.
What should I ask my clinician before starting this insulin?
Ask how and when to use the insulin, what blood glucose range you should monitor for, and what to do if meals, activity, illness, or other medicines change. You can also ask whether the vial is intended for syringe use, pump use, or another setup. Confirm how to treat low blood sugar and when to contact your care team.
Can a vial be used with an insulin pump?
Some people use rapid-acting insulin lispro in an insulin pump, but pump use depends on the prescribed care plan and the device instructions. The pump manufacturer may specify which insulins and reservoirs are compatible. Do not place insulin in a pump unless your clinician has prescribed that use and you understand the backup plan for pump interruption or unexplained high glucose.
Rewards Program
Earn points on birthdays, product orders, reviews, friend referrals, and more! Enjoy your medication at unparalleled discounts while reaping rewards for every step you take with us.
You can read more about rewards here.
POINT VALUE
How to earn points
- 1Create an account and start earning.
- 2Earn points every time you shop or perform certain actions.
- 3Redeem points for exclusive discounts.
You Might Also Like
Related Articles
How to Get Retatrutide: Legal Access and Safety Checks
Retatrutide access depends first on regulatory approval. If you are searching for how to get retatrutide, start by checking whether a regulator has approved a specific product where you live.…
Continuous Glucose Monitoring: How CGMs Fit Diabetes Care
Continuous glucose monitoring is a way to track glucose throughout the day and night with a small wearable sensor. It matters because it shows patterns, direction, and alerts that a…
How to Get Rid of a Cold Sore and Ease Symptoms Safely
A cold sore usually cannot be erased overnight. If you want to know how to get rid of a cold sore, the fastest practical step is to treat it early,…
What Is Glucagon Like Peptide 1 and What Does It Do?
What is glucagon like peptide 1? In simple terms, it is a hormone your gut releases after you eat. Clinically, it is called glucagon-like peptide-1, or GLP-1, an incretin (a…