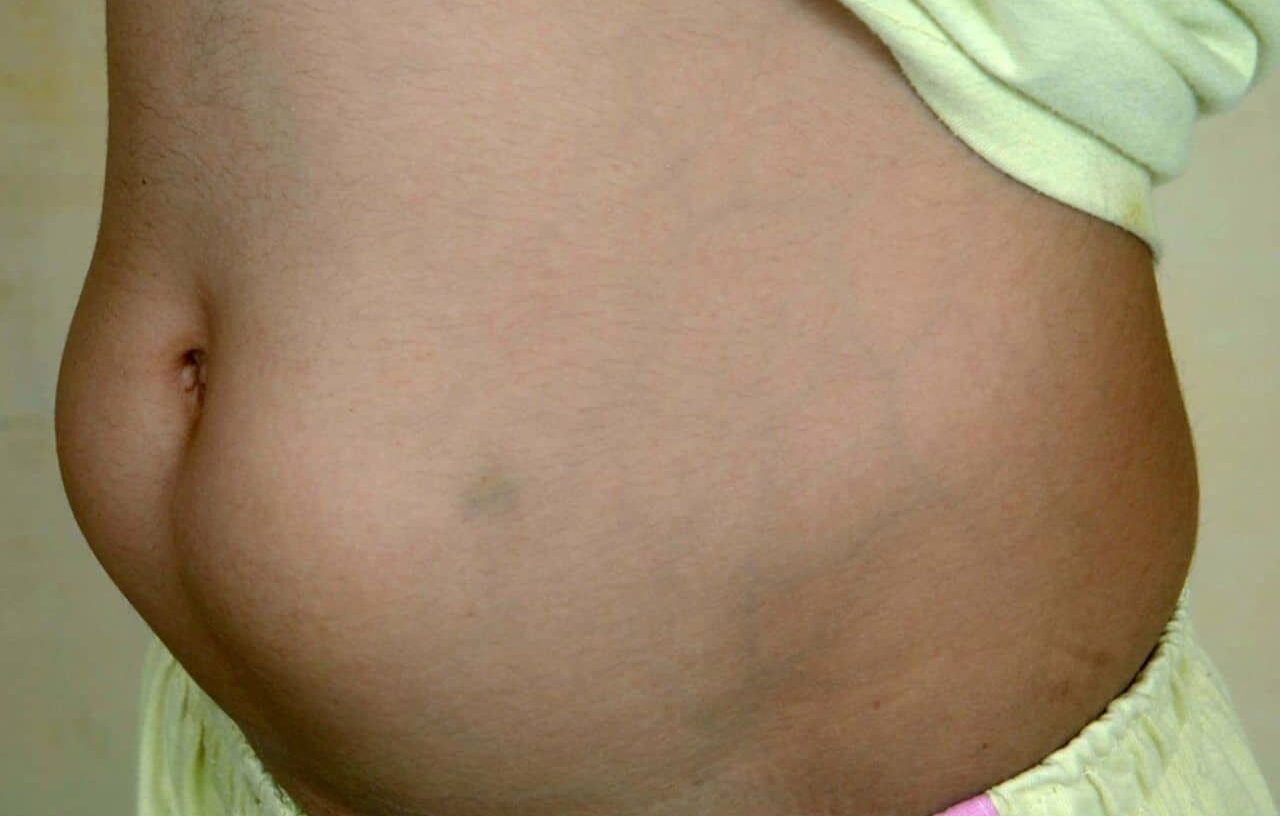
Lipohypertrophy is a thickened, rubbery, or lumpy area of subcutaneous (under-the-skin) fat that usually develops after repeated insulin injections or pump infusions in the same small spot. It matters because insulin may absorb less predictably from affected tissue, which can make glucose patterns harder to interpret. The issue is most often discussed in people who use insulin, but the core problem is repeated local tissue stress over time.
Key Takeaways
- Lipohypertrophy usually develops from repeated injections or infusions in the same small area.
- It may feel like a lump, firm patch, or thickened area under the skin.
- Affected tissue can change how insulin absorbs and may contribute to erratic glucose patterns.
- Rotation, site checks, and avoiding damaged areas are the main prevention steps.
- Redness, warmth, drainage, severe pain, or a fast-changing mass need medical review.
What Lipohypertrophy Is and Why It Matters
Lipohypertrophy is a local tissue change, not just a cosmetic bump. It tends to form in areas used again and again for insulin delivery. People living with Diabetes and some people with Type 2 Diabetes may notice it in the abdomen, thighs, arms, or other approved injection regions. Sometimes the area looks raised. Other times it is easier to feel than to see.
The main concern is not appearance alone. Insulin is meant to move from the fat layer under the skin into the bloodstream at a reasonably consistent pace. When that tissue becomes thickened or uneven, absorption can become less predictable. That is one reason site checks matter alongside understanding the Role Of Insulin in glucose control.
Why it matters: Using an affected site can make glucose readings less predictable.
Clinicians usually identify lipohypertrophy by looking at the area, feeling for firmness or thickness, and asking about injection habits. Diagnosis is often based on history and exam rather than one special test. Many people casually call it scar tissue, but the change is usually a buildup or thickening in the fat layer rather than a simple surface scar. Scar-like tissue can still coexist, especially after years of repeated punctures.
Common Causes and Risk Factors
The most common cause is repeated insulin delivery into the same small zone. A person may think they are rotating because they switch left to right or move only slightly each day, yet still return to the same favorite patch of skin. Over time, that repeated local trauma and insulin exposure can contribute to tissue growth and thickening.
This can happen with syringes, pens, and insulin pump infusion sets. If you use devices across Pens, Pumps, And CGMs, it helps to remember that pump sites deliver insulin while a CGM sensor tracks glucose. A CGM sensor is not usually the direct cause of lipohypertrophy, though it can cause other local skin reactions. People browsing Insulin Options may focus on the medication itself and overlook how much site selection affects day-to-day use.
Risk tends to rise when rotation is inconsistent, the same spot hurts less and becomes a habit, the skin is not checked routinely, or needles and site components are reused beyond instructions. Convenience also plays a part. One easy-to-reach area can become the default site for weeks. Long-term insulin therapy increases exposure simply because there are more opportunities for repetition.
The problem is not limited to one diabetes type. Adults using Type 2 Diabetes And Insulin can develop the same tissue changes as people with type 1 diabetes. The basic pattern is the same: repeated insulin delivery into a narrow area instead of rotating across healthy tissue.
Prescription details may be confirmed with the prescriber when needed.
What It May Look and Feel Like
Lipohypertrophy may feel soft, firm, rubbery, or thick compared with nearby skin. Some areas feel like a flat plaque rather than a round lump. Others look puffy, swollen, or uneven. In many cases, injections into that spot hurt less, which can unintentionally encourage a person to keep using it.
- Raised or puffy patch under the skin
- Firm or rubbery area that feels different
- Thickened skin or a dense fatty lump
- Reduced sensation during injections
- A familiar spot that seems easier to use
- Unexplained glucose swings after using that area
Online photos can give a rough idea, but lipohypertrophy pictures do not always capture subtle cases. Some tissue changes are easier to find by touch. That is why clinicians and diabetes educators often check sites with both inspection and gentle palpation.
How to check injection sites
Look at the skin in good light, then feel across the area with slow, light pressure. Compare both sides of the body if you use paired areas. You are looking for differences in thickness, firmness, texture, or sensitivity, not just obvious lumps. If site changes seem to match swings seen on Blood Glucose Monitors or Test Strips, note that pattern before your next visit. A simple record of body site, time, and reading can make the pattern easier to spot.
If you find a suspicious area, do not keep injecting there just because it feels easier. Mark it mentally or on a rotation map and bring it up with a clinician, nurse, or diabetes educator. They can often tell whether the area fits with lipohypertrophy or whether another problem should be considered.
Lipohypertrophy vs Lipoatrophy and Other Site Changes
Lumps at injection sites do not all mean the same thing. People often use the term scar tissue loosely, but several different skin or fat-layer changes can happen with injections. A quick comparison helps explain why the appearance, feel, and timing matter.
| Change | Typical look or feel | Why the distinction matters |
|---|---|---|
| Lipohypertrophy | Raised, thickened, rubbery, or lumpy fatty tissue | Insulin absorption may become less predictable, so affected areas are usually avoided. |
| Lipoatrophy | Loss of fat that leaves a dent or hollow area | This is a different tissue change and may call for a separate review of technique or treatment factors. |
| Bruising or mild irritation | Discoloration, tenderness, or a short-lived sore spot | These changes are often more temporary than a persistent fatty lump. |
| Possible infection or inflammation | Red, hot, painful, draining, or rapidly changing area | This needs prompt medical assessment rather than simple site rotation alone. |
This comparison is general, not a diagnosis. A clinician may still need to examine the area, especially if there is pain, warmth, skin breakdown, or a rapid change in size. It also helps to mention how long the change has been there and what device or injection pattern you were using when it appeared.
How to Prevent Lipohypertrophy
Prevention centers on rotation, inspection, and consistent technique. The goal is not only to switch body regions from time to time, but also to avoid using the exact same point within one region. Approved injection or infusion sites vary by product and device, so the specific instructions still matter. What stays consistent is the need to spread out local skin stress.
People often fall into patterns because one area is easy to reach, works well under clothing, or feels less painful. A simple rotation plan helps break that cycle. Many people keep site notes with other Diabetes Supplies so the routine stays visible instead of becoming guesswork.
- Plan the week ahead and map a simple rotation pattern.
- Leave space between punctures instead of clustering one small area.
- Look and feel before each injection or site change.
- Avoid any lump, firm patch, or numb area.
- Use fresh needles or site components as directed.
- Review technique if readings become harder to predict.
- Change pump infusion zones regularly, not just the exact set.
Quick tip: A phone note or body diagram can make rotation easier to follow.
Prevention also means acting early. If an area starts to feel different, resting it is often more useful than trying to push through. If glucose patterns change, a technique review may matter before assuming the medication dose is the only issue. Small errors in spacing, site choice, or repeated use of one comfortable zone can add up over time.
No single routine fits everyone. Children, older adults, people with reduced dexterity, and people who rely on one easy-to-reach body area may all need a more deliberate plan. A clinician or diabetes educator can help match rotation habits to the specific pen, syringe, or pump method you use.
Can Lipohypertrophy Go Away?
Lipohypertrophy may improve after the area is rested, but it does not always disappear quickly. Some lumps flatten over time. Others remain noticeable for longer, especially if they were used repeatedly for a long period. That is why early detection matters. Smaller or newer changes may be easier to manage than long-standing ones.
There is no standard cream that reliably removes the tissue change. The main management step is usually to stop using the affected area and switch to healthy sites. Massage, rubbing, or home remedies are not standard solutions. What helps most is avoiding further trauma, reviewing technique, and giving the tissue time away from injections or infusions.
A clinician or diabetes educator can help confirm the finding, map safer alternatives, and review technique so the problem does not keep recurring. They may also ask whether you have seen more unexplained highs or lows after injections. If that pattern sounds familiar, reviewing the basics of Hypoglycemia Vs Hyperglycemia can help you describe what is happening more clearly.
Dispensing is handled by licensed third-party pharmacies where permitted.
When to Seek Medical Review
You should seek medical review sooner if the area is red, hot, very painful, draining, rapidly growing, or associated with fever. Those features suggest something more than routine lipohypertrophy. A hard fixed mass, major color change, or skin ulceration also deserves prompt evaluation.
Even without those warning signs, it is worth asking for help if glucose control becomes harder to explain, injections suddenly feel very different, or you are no longer sure where to place your next dose. A routine site exam can sometimes solve weeks of confusion. Many people do not realize how much one overused spot can affect day-to-day patterns until the area is checked.
If you are unsure whether a pump site, pen injection pattern, or general technique issue is involved, bring your device notes or rotation record to the visit. Small details often matter. A brief site check can show whether the problem is a local tissue change, a technique issue, or a separate skin condition that needs different care.
Authoritative Sources
- For patient-friendly prevention basics, review MyHealth Alberta on preventing lipohypertrophy.
- For professional diabetes education context, see ADCES on lipohypertrophy.
- For a detailed evidence review, read this peer-reviewed review on lipohypertrophy and insulin.
Further reading: Lipohypertrophy is often preventable, and regular site checks can make insulin use easier to interpret and discuss with your care team.
This content is for informational purposes only and is not a substitute for professional medical advice.