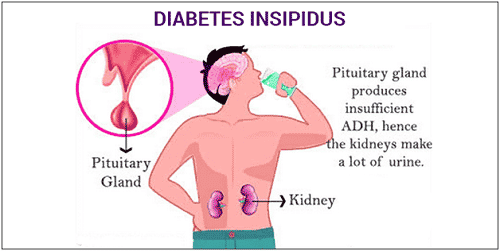
Central diabetes insipidus is a rare disorder caused by too little vasopressin, also called antidiuretic hormone (ADH), from the hypothalamus or posterior pituitary. Without enough hormone, the kidneys cannot conserve water well, so a person passes large volumes of very dilute urine and becomes intensely thirsty. This matters because untreated water loss can lead to dehydration, high sodium levels, and confusion, especially after pituitary surgery, head injury, or illness affecting the brain. The condition is also called neurogenic or cranial diabetes insipidus, and despite the name, it is different from diabetes mellitus, which involves blood sugar.
Key Takeaways
- It is a water-balance disorder caused by impaired vasopressin production or release.
- Common causes include pituitary surgery, tumors, head injury, and disorders affecting the hypothalamus or pituitary.
- Main symptoms are excessive urination, constant thirst, nighttime urination, and dehydration risk.
- Diagnosis often uses blood and urine testing, supervised water deprivation testing, desmopressin response, and MRI.
- Treatment usually centers on desmopressin, treating the underlying cause when possible, and monitoring sodium and fluid balance.
What Central Diabetes Insipidus Means
Central diabetes insipidus starts in the brain rather than the kidneys. Under normal conditions, the hypothalamus makes vasopressin and the posterior pituitary stores and releases it when the body needs to conserve water. If that signal is reduced or absent, the kidneys let too much free water pass into urine. The result is polyuria (passing unusually large amounts of urine) and polydipsia (excessive thirst).
Vasopressin works mainly at the collecting ducts in the kidneys, where it tells the body to reclaim water instead of wasting it. When that message is missing, urine stays very dilute even when the body is short on fluids. The thirst center often tries to compensate, which is why many people feel driven to drink again and again. In rare situations, thirst may also be impaired, and that makes dehydration risk much higher.
This is why the condition can feel relentless. A person may carry water everywhere, wake several times each night to urinate, or notice symptoms become far more serious during fasting, illness, or travel. Because drinking can temporarily offset the water loss, diagnosis is sometimes delayed until a hospital stay, surgery, or another stressful event disrupts normal access to fluids.
The name also causes confusion. Diabetes insipidus is not a blood sugar disorder. It sits within the broader world of hormone and fluid regulation, so it helps to view it alongside the Diabetes And Endocrine System. Still, its biology, testing, and treatment are different from the more familiar forms of diabetes mellitus.
Why it matters: Severe water loss can raise sodium quickly and become a medical emergency.
Common Causes And When It Appears
Most cases happen after damage, inflammation, or pressure affecting the hypothalamus or pituitary region. That includes pituitary or skull-base surgery, tumors near the pituitary stalk, head trauma, and some infiltrative or inflammatory disorders. Less often, infections or inherited conditions are involved. In some people, no clear cause is found even after testing.
After Surgery Or Head Injury
Symptoms can begin abruptly after pituitary surgery, neurosurgery near the base of the brain, or a significant head injury. In that setting, urine output may rise over hours rather than weeks. That is one reason hospitals often watch fluid intake, urine volume, and sodium levels closely after these events. Early changes can be subtle until dehydration becomes more obvious.
Not every postoperative case is permanent. Some people develop short-lived hormone disruption from swelling or temporary injury, then improve as healing progresses. Others have persistent disease when the vasopressin pathway has been more substantially damaged. The pattern is not always obvious on day one, so follow-up matters.
Other Structural And Medical Causes
Tumors involving the hypothalamus, pituitary gland, or pituitary stalk can interfere with hormone production, storage, or release. Inflammatory and infiltrative disorders may do the same. In children, clinicians may also consider congenital brain or pituitary abnormalities, though the condition remains uncommon overall.
A separate condition, gestational diabetes insipidus, can occur during pregnancy because of changes in hormone breakdown. It is not the same as a central form, even though the symptoms can overlap. That distinction matters because the timing, cause, and workup differ.
Because the pituitary influences several other hormones, clinicians often look beyond thirst and urination alone. Headaches, vision changes, fatigue, menstrual changes, low libido, or slowed growth in children can offer clues that a broader pituitary or hypothalamic problem is present.
Symptoms And Complications To Watch For
The classic pattern is passing large amounts of very dilute urine and feeling unable to drink enough water. Symptoms often sound straightforward at first, but the consequences can become serious when fluid losses outpace intake.
- Excessive urination: large urine volumes, often pale or clear.
- Constant thirst: strong need for water, sometimes all day and night.
- Night waking: repeated urination can disrupt sleep.
- Dryness and fatigue: dehydration may cause dry mouth, dizziness, and weakness.
- Neurologic changes: confusion, drowsiness, or seizures can occur with severe sodium imbalance.
Daily life can be affected long before an emergency develops. Many people notice constant planning around bathrooms, poor sleep from nocturia, dry mouth, headaches, and trouble concentrating. When symptoms increase suddenly after surgery or injury, clinicians pay closer attention because sodium can shift faster in those settings.
Infants and young children may not describe thirst clearly. Instead, they may show irritability, poor feeding, fever, constipation, bedwetting, slow growth, or unexplained dehydration. Older adults and people with cognitive impairment can also be vulnerable because they may not recognize or respond to thirst as reliably.
Hypernatremia, meaning a high sodium level, is a major complication of untreated or undertreated disease. Urgent assessment is especially important when intense thirst or heavy urination is paired with vomiting, major weakness, fainting, confusion, reduced alertness, or inability to access water. Those signs may mean the body is no longer keeping up with fluid losses.
Quick tip: Bring a short log of thirst, nighttime urination, and major fluid changes to appointments.
How Central Diabetes Insipidus Is Diagnosed
Diagnosis starts by confirming excessive water loss and then asking why it is happening. Doctors usually begin with symptom history, exam findings, and blood and urine testing. Very dilute urine, especially alongside a rising sodium or blood osmolality level, can point toward diabetes insipidus rather than a routine hydration problem.
Testing may include urine specific gravity, urine osmolality, serum sodium, and blood osmolality. In some cases, a 24-hour urine collection helps quantify how much urine is being produced. The goal is not only to show that urination is frequent, but to show that the body is losing too much free water.
The next step is separating a central cause from nephrogenic diabetes insipidus, where the kidneys do not respond properly to vasopressin, and from primary polydipsia, where very high fluid intake is the main driver. A supervised water deprivation test may be used in selected cases. During that test, clinicians watch how urine concentration changes when fluids are withheld under controlled conditions. Because dehydration and sodium shifts can become dangerous, this is not a test to attempt at home.
A desmopressin response test can add another clue. If urine becomes more concentrated after desmopressin, that pattern supports a central problem rather than kidney resistance. MRI is often used to examine the hypothalamus and pituitary for tumors, inflammation, postoperative changes, or stalk abnormalities. Many patients also need a review of other pituitary hormones because disorders in this area do not always occur alone.
Getting the label right matters. Treating repeated dehydration episodes without identifying the hormone problem can miss the reason symptoms keep returning. It can also delay treatment of an underlying pituitary lesion or another brain disorder that needs separate attention.
Treatment And Monitoring For Central Diabetes Insipidus
Treatment usually focuses on replacing the missing hormone effect and keeping water balance stable. Desmopressin, a vasopressin analog, is the main prescription therapy for many people with central diabetes insipidus. The exact regimen is individualized. The goal is not simply to stop urine output, but to reduce excessive water loss without pushing the body toward water retention.
Watching For Under And Over-Treatment
Monitoring is as important as the prescription itself. Too little treatment can leave a person dehydrated and hypernatremic. Too much can cause water retention and hyponatremia, meaning sodium becomes too low. That is why clinicians often review symptom patterns, sodium levels, urine output, and changes in routine such as illness, fasting, or recent surgery.
These swings can feel confusing because both under-treatment and over-treatment can cause a person to feel unwell. Persistent thirst, rising urine output, dry mouth, and weakness can suggest inadequate control. On the other hand, new headaches, nausea, swelling, or unexpected fatigue can raise concern for too much water being retained. Interpretation depends on the wider clinical picture, not one symptom alone.
Higher-Risk Situations
Children, older adults, hospitalized patients, and people with reduced thirst sensation may need closer supervision because they may not compensate for water loss as reliably. The same is true around surgery, vomiting, diarrhea, prolonged fasting, and severe illness. In those periods, plans for fluid intake, lab checks, and follow-up often matter more than during a stable week at home.
Some people also need treatment for the underlying cause. That may include follow-up after pituitary surgery, evaluation of a brain lesion, or management of another endocrine disorder. Long-term care often involves endocrinology follow-up, especially when other pituitary hormones are affected or when MRI findings need to be tracked over time.
Platform note: Prescription details may be confirmed with the prescriber when required.
Living With The Condition Day To Day
Daily management is usually about knowing your pattern rather than reacting to every bathroom trip. Many people do well once the diagnosis is clear and treatment is stable, but symptoms can return quickly when routines change. Illness, fasting, travel, and postoperative recovery are common times when extra planning matters.
Practical preparation can make a real difference. People often ask how to handle long car rides, school or work schedules, airline travel, or procedures that require not eating or drinking. The most useful answers are usually individualized and focus on safe access to water, when to contact the care team, and how to avoid long stretches without fluids when symptoms are active.
Caregivers play an important role when the patient is a child, an older adult, or someone who cannot reliably report thirst. A simple care plan may include symptom tracking, bathroom patterns, recent illnesses, and a list of questions for follow-up visits. Outlook depends in part on the cause. Temporary cases may improve, while chronic cases often need ongoing monitoring and periodic reassessment.
Central Vs Nephrogenic Diabetes Insipidus And Diabetes Mellitus
These conditions can all involve thirst and frequent urination, but the source of the problem is different. Central diabetes insipidus reflects low or absent vasopressin production or release. Nephrogenic disease means vasopressin is present, but the kidneys do not respond properly. Diabetes mellitus is driven by glucose regulation problems involving insulin and related metabolic pathways.
| Condition | Main problem | Typical urine pattern | Common diagnostic direction |
|---|---|---|---|
| Central DI | Too little vasopressin from the hypothalamus or pituitary | Large volumes of dilute urine | Blood and urine testing, desmopressin response, MRI |
| Nephrogenic DI | Kidneys resist vasopressin | Large volumes of dilute urine | Evaluation of kidney response, medication causes, inherited or acquired factors |
| Diabetes mellitus | Glucose regulation disorder | Urination may increase when blood sugar is high | Blood glucose and A1C testing, related metabolic assessment |
This distinction matters because the same symptom can point to very different problems. Nephrogenic forms may relate to kidney disease, certain medications, or inherited factors. In diabetes mellitus, high blood sugar causes osmotic diuresis, meaning glucose pulls water into urine. If you want a broader refresher on glucose-based conditions, see Other Types Of Diabetes and What Is Ketonuria. The name overlap causes frequent confusion, but the biology and treatment path are not the same.
What To Track Between Visits
The most useful record is usually a simple log rather than a detailed spreadsheet. A few consistent notes can help an endocrinologist see whether symptoms are stable, worsening, or changing with treatment.
- Urination pattern: daytime frequency and overnight waking.
- Thirst level: whether drinking feels manageable or relentless.
- Weight shifts: sudden drops can reflect water loss.
- Illness or fasting: vomiting, procedures, or missed fluids.
- New symptoms: headaches, vision changes, or confusion.
- Medication changes: anything that may affect fluids or kidneys.
It also helps to ask how often sodium should be checked, when repeat imaging is needed, and which symptoms should trigger urgent evaluation. For broader hormone-related reading, browse the Endocrine Thyroid Hub. Another example of endocrine overlap is Osteoporosis And Diabetes, which shows how hormone disorders can intersect even when the mechanism is very different.
Platform note: Dispensing is handled by licensed third-party pharmacies where permitted.
Authoritative Sources
- For a broad patient overview, see Mayo Clinic on Diabetes Insipidus.
- For kidney-focused background and definitions, review the NIDDK Diabetes Insipidus page.
- For hospital safety details, read the Society for Endocrinology Guideline.
Central or neurogenic diabetes insipidus is a water-balance disorder tied to vasopressin deficiency. The key tasks are identifying the cause, distinguishing it from look-alike conditions, and monitoring treatment carefully over time. Further reading can help, but sudden confusion, marked weakness, or inability to keep up with fluid losses needs prompt medical attention.
This content is for informational purposes only and is not a substitute for professional medical advice.