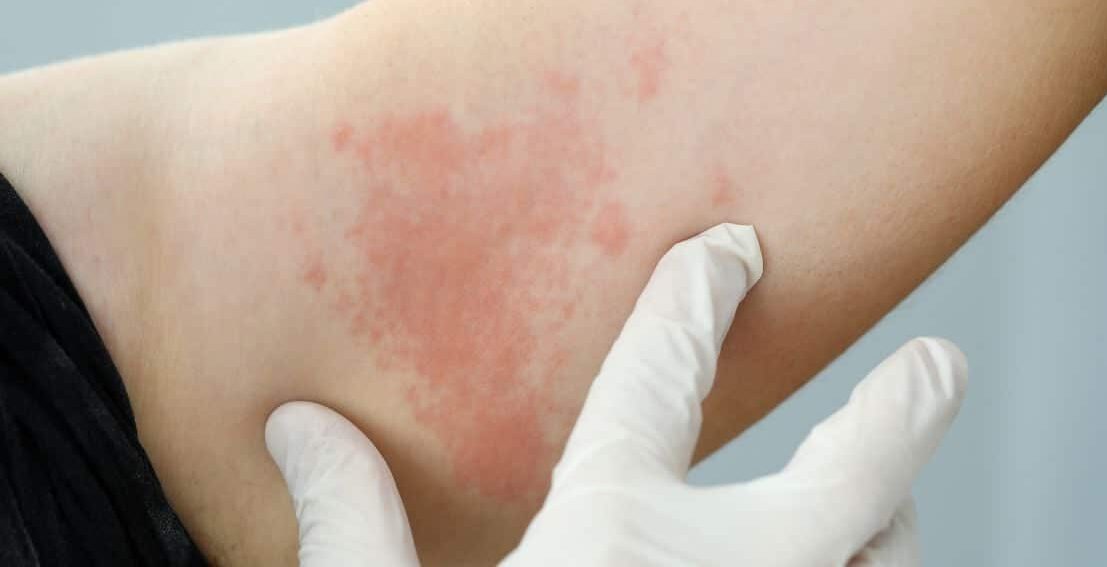
Skin can signal how well diabetes is controlled. Diabetes Skin Problems often reflect changes in blood flow, immune response, and nerve function. Recognizing early signs helps you prevent infections, protect your feet, and discuss concerns promptly with your clinician.
Key Takeaways
- Common patterns: dry skin, shin spots, yeast rashes, and foot fungus.
- Early care: moisturize, protect skin barriers, treat infections quickly.
- Red flags: spreading redness, fever, ulcers, or black tissue.
- Control matters: stable glucose reduces most inflammatory flares.
Diabetes Skin Problems: Causes and Common Patterns
Diabetes influences skin through several pathways. High glucose promotes dryness (xerosis), reduces immunity, and impairs microvascular flow. Nerve damage (neuropathy) reduces sweating on lower legs and feet, which dries the skin and increases fissures. These changes make minor injuries and fungal infections more likely, especially between toes and on the soles.
Several recognizable conditions appear more often in diabetes. These include shin spots called diabetic dermopathy, velvety darkening on the neck known as acanthosis nigricans, and candida rashes in skin folds. For a broader overview of skin changes, see How Diabetes Affects Your Skin to understand how glucose control influences the skin barrier.
Clinicians emphasize risk reduction alongside treatment. Keep nails trimmed, avoid barefoot walking, and check pressure points daily. When skin breaks do occur, cleanse gently and cover with a breathable dressing. For storage and hygiene tips related to sweat and irritation management, see Diabetes And Sweating for context on moisture control.
Recognizing Lesions on Legs and Feet
The lower legs and feet face the greatest friction and pressure. Many people notice round, light brown shin patches with a thin, scaly surface. These are often benign shin spots. Others develop ring-shaped rashes on the feet from tinea pedis (athlete’s foot), which may crack the skin and invite bacteria.
A diabetic rash on legs may present as itchy plaques, ring-like fungal patches, or clusters of small red bumps. Pay attention to warmth, swelling, or drainage, which can signal bacterial infection. For guidance on how skin breakdown slows recovery, see Diabetes And Wound Healing because impaired healing changes infection risk. For antifungal options used on the feet, see Terbinafine for typical indications and use discussions.
Foot care protects long-term mobility. Seek help for any ulcer, new numbness, or color changes. For context about severe limb complications and prevention strategies, see Why Do Diabetics Lose Limbs to understand foot risk factors and protective steps.
Diabetic Dermopathy vs Other Conditions
Shin spots usually appear as painless, oval-to-round, light brown patches with a shiny surface on the shins. They often follow minor trauma and gradually fade. When clinicians discuss diabetic dermopathy symptoms, they emphasize asymptomatic, flat patches that do not ulcerate. These marks rarely require treatment, though their presence may correlate with long-standing diabetes and microvascular changes.
Not all leg lesions are the same. Necrobiosis lipoidica (collagen degeneration) can create yellowish plaques with a red rim, sometimes on the shins. These may become thin and fragile. Because heavy inflammation and ulceration can occur, prompt evaluation is important. For a concise clinical overview of shin changes, the DermNet guidance offers descriptive features and differential points. When patches appear alongside rising glucose, see Signs Of Uncontrolled Diabetes to review systemic indicators that may parallel skin changes.
How It Differs From Other Shin Conditions
Dermopathy tends to be flat, light brown, and non-tender. Stasis dermatitis from venous issues often looks red-brown with swelling and itch near the ankles. Tinea corporis (ringworm) shows a scaly, advancing border with central clearing. Necrobiosis lipoidica may appear waxy or atrophic centrally and can ulcerate after minor trauma. Documenting lesion size, color, and border helps your clinician separate these patterns. Good photos taken in consistent lighting can aid comparisons during follow-up.
Itching, Rashes, and Early Management
Itch (pruritus) in diabetes often stems from dry skin, yeast overgrowth, or neuropathy. Start with gentle, fragrance-free cleansers. Take short, lukewarm showers and moisturize within three minutes using a thick cream or ointment with urea or ceramides. A cool compress can settle inflamed areas.
When learning how to relieve diabetic itching, address triggers first: dryness, friction, or sweat. Consider non-sedating antihistamines for generalized itch if your clinician agrees. Use low-potency topical corticosteroids briefly for inflamed, noninfected rashes; avoid steroids on suspected fungal areas. For perspiration-related intertrigo in folds, see Diabetes And Sweating for practical moisture control steps. If yeast involvement is likely, topical azoles may help; for examples and precautions, see Ketoconazole to understand common uses and cautions.
Evidence-based guidance highlights skin care and glucose control. The American Diabetes Association notes that moisturization and infection control reduce complications; see their overview of skin care in diabetes for patient-facing best practices. The NIH’s MedlinePlus on diabetes and skin problems provides condition summaries and general measures.
When to Seek Care and What Tests Help
Escalate care for spreading redness (cellulitis), warmth, tenderness, or fever. Black, blue, or rapidly expanding areas can indicate tissue loss or vascular compromise. New ulcers, persistent drainage, or a foul odor require prompt clinical evaluation. Sudden numbness, cold toes, or calf pain with walking warrant vascular assessment.
People often ask, is diabetic dermopathy dangerous? Dermopathy is usually benign, but it can coexist with circulation or nerve issues that deserve attention. Clinicians may check glucose, A1C, and perform skin scrapings with KOH for fungus or culture if discharge is present. For urgent system-wide symptom patterns, see Diabetes Attack Symptoms to understand when immediate evaluation is warranted. The CDC offers general guidance on managing diabetes problems, which includes prevention strategies relevant to skin health.
Treatment Pathways and Skin Care Plan
Tailor treatment to diagnosis and severity. Bacterial infections may require prescription antibiotics after clinical assessment. Fungal infections on the feet often respond to topical agents used consistently for several weeks. For oral therapy details that clinicians may consider, see Fluconazole for indications and monitoring notes. Protect fragile skin with emollients and reduce friction with well-fitted footwear.
Regarding diabetic dermopathy treatment, evidence suggests lesions usually fade without direct therapy; focus on glucose stability and leg protection. Some inflammatory dermatoses may be managed with calcineurin inhibitors when appropriate; for clinical context, see Tacrolimus HGC as an example product that clinicians use in selected conditions. For additional topical options and counseling points, review Ketoderm to compare azole formulations used for yeast or dermatophytes.
Tip: Keep a simple routine: gentle cleanser, thick moisturizer, targeted prescription when indicated, and regular foot checks. Minimal products reduce irritation risk and improve adherence.
Visual Pattern Cues and What Photos Show
Photos can help you track change, but they cannot diagnose. High-quality images taken in natural light can reveal scale, color, and border. Review for ring-like edges (fungus), bright red moist patches (yeast), or flat brown shin spots (dermopathy). If a lesion looks different, grows, or becomes tender, schedule a timely evaluation.
People often search for diabetic skin conditions pictures to compare patterns. Use reputable sources and avoid overinterpreting color differences from lighting. Document size with a ruler and note symptoms like itch or pain. For complementary reading across dermatology topics, browse Dermatology Articles because visual descriptions there can support your understanding of common presentations.
Pre-Diabetes Skin Signs and Prevention
Insulin resistance may cause acanthosis nigricans (velvety darkening) on the neck and underarms, plus skin tags on friction areas. Dryness and mild folliculitis can also appear. While there is no single pre diabetes diabetic rash, clusters of these findings with weight gain or fatigue should prompt metabolic screening. Early nutrition, activity, and weight management steps can improve skin comfort and cardiometabolic health.
Prevention starts with basics: hydration, sun protection, and daily foot inspection. Wear moisture-wicking socks and rotate shoes to limit fungal growth. For curated reading on metabolic health and skin, see Diabetes Articles because related guides outline broader prevention strategies that also safeguard skin.
Recap
Skin changes in diabetes often reflect dryness, friction, infections, and microvascular shifts. Most rashes improve with barrier care, targeted treatment, and consistent glucose control. Pay attention to legs and feet, where pressure and neuropathy concentrate risk. Seek care early for spreading redness, ulcers, or tissue discoloration.
Use consistent routines, document lesion changes, and prioritize comfortable footwear. When unsure, conservative care and timely evaluation are safer than waiting. With steady habits and informed monitoring, most skin issues can be managed effectively over time.
This content is for informational purposes only and is not a substitute for professional medical advice.