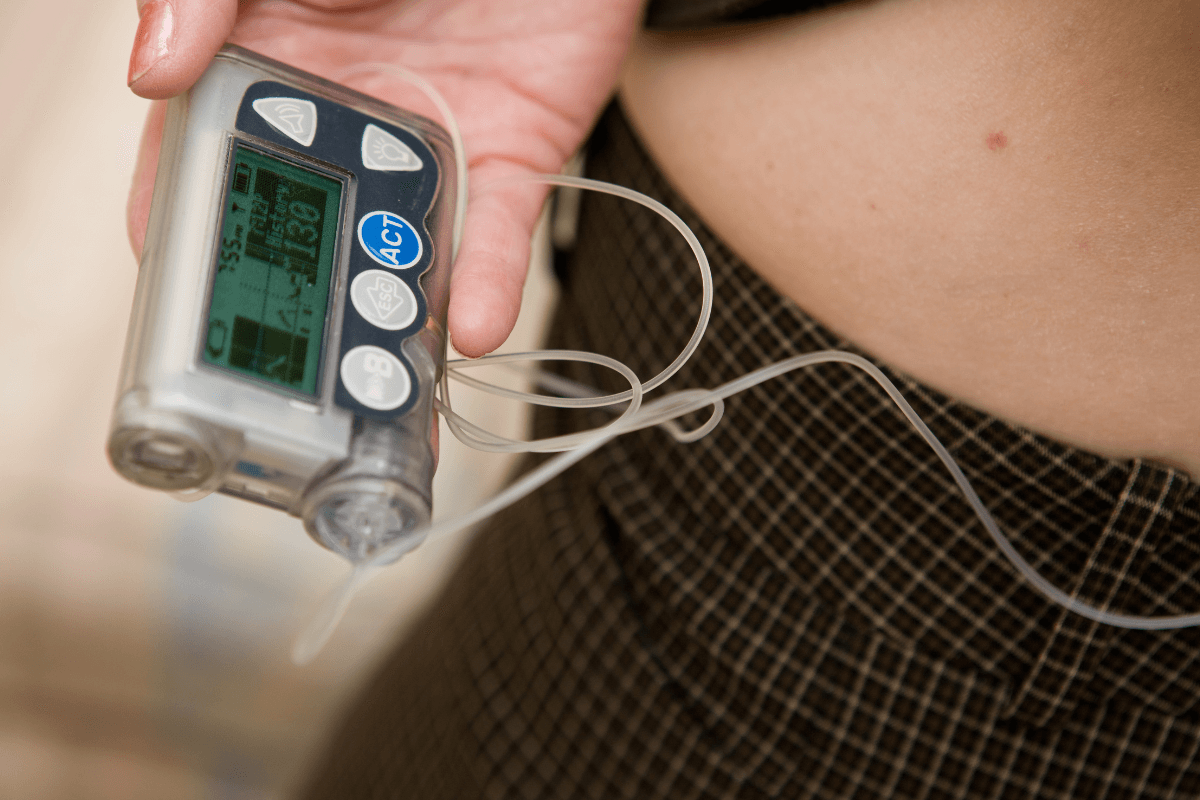
The Humalog insulin pump allows rapid-acting insulin lispro to be delivered in precise, programmable amounts. It can help smooth daily glucose patterns when used with accurate settings and consistent monitoring.
Key Takeaways
- Rapid-action basal and bolus: continuous microdoses plus mealtime doses.
- Compatibility matters: use U-100 lispro approved for pump delivery.
- Dose safety: confirm ratios, sensitivities, and active insulin tracking.
- Device trade-offs: tubing, alarms, and occlusion risks require backup plans.
Humalog Insulin Pump: Core Mechanics and Compatibility
Insulin pumps deliver a background basal rate and user-triggered boluses through an infusion set. With lispro, onset and offset are relatively fast, which helps match meal absorption and correction dosing. Many users describe steadier fasting levels once basal rates are tuned across 24 hours. Accuracy depends on site quality, set integrity, and timely reservoir changes.
Compatibility and infusion-set guidance are described in the Humalog prescribing information. Only the U-100 formulation is intended for continuous subcutaneous infusion. Use reservoirs, cannulas, and change intervals recommended by your device manufacturer. For pump basics and terminology, see What Is an Insulin Pump for a plain-language walkthrough. For lispro pharmacology in meal coverage, the overview in Humalog Vial Rapid Insulin highlights its rapid onset characteristics.
What Type of Insulin Works in Pumps
The short answer to what type of insulin is used for insulin pump therapy is rapid-acting analogs. Pumps typically use insulin lispro (Humalog), insulin aspart (NovoRapid), or insulin glulisine (Apidra). These formulations start quickly and clear within several hours, which reduces stacking when timing and tracking are careful. Regular human insulin is seldom used in modern pumps because of slower kinetics.
If aspart is preferred, the cartridge format in NovoRapid Cartridge may align with your device’s fill process. For clinical context on glulisine, see Understanding Apidra Insulin and compare onset/offset with lispro. Broader guidance on insulin delivery appears in the ADA Standards of Care, which discuss pump suitability and monitoring.
Basal–Bolus Dosing and Daily Use
Effective programming aligns basal rates to physiologic needs by clock hour. Mealtime boluses combine carbohydrate coverage with a correction factor when needed. The goal is to prevent peaks and dips by matching insulin action to food absorption and activity. Tracking insulin on board helps avoid stacking.
Discuss insulin infusion pump dosage principles with your care team before changing any settings. Typical workflows include insulin-to-carb ratios, insulin sensitivity factors, and pre-bolus timing for higher-glycemic meals. A continuous glucose monitor can reveal dawn rises or late drops and guide refinements. For structured decision steps, see Bolus Insulin Dosing and how technology pairs across systems in Diabetes Tech Overview.
Tip: When testing basal rates, choose low-variability periods and document activity, meals, and correction-free intervals for cleaner interpretation.
Who Benefits and Common Trade-Offs
Pumps can help people who want fewer daily injections, flexible scheduling, and programmable profiles for shifts or weekends. They may also help reduce glycemic variability by tailoring basal rates and using extended or dual-wave boluses for higher-fat meals. Integration with continuous glucose monitoring can add alerts and insulin-suspension features in certain systems.
Common disadvantages of insulin pump include device wear, infusion-set failures, skin irritation, and a learning curve for settings. Tubing and adhesives can complicate sports or water exposure. If a rapid-acting alternative fits better for you, compare options in Novolog vs Humalog to understand pharmacologic differences and practical trade-offs.
Safety, Side Effects, and Set Issues
Known humalog insulin side effects include hypoglycemia, infusion-site reactions, and potential hypokalemia in predisposed patients. Pump-specific risks include rapid hyperglycemia and ketosis if delivery is interrupted, because only rapid-acting insulin is on board. Rotate sites to reduce lipodystrophy (fat changes under the skin), and replace sets on schedule to limit occlusions.
Serious allergic reactions are uncommon but require urgent care. Cardiovascular events are not typical with lispro alone, and hair loss is not a listed common adverse event in product labeling. The label also clarifies that U-200 lispro is not intended for pump use, which helps avoid concentration errors. For formal safety details, review the Humalog prescribing information; practical pump cautions are also summarized in Diabetes Canada’s insulin therapy guidance.
Pumps vs Pens and Cartridges
Pens and pumps both deliver rapid-acting insulin but differ in workflow. Pumps excel at nuanced basal control, while a humalog insulin pen may be simpler for people preferring injections. Cartridges and reusable devices can reduce waste and allow finer dialed doses without wearing hardware 24/7. Consider lifestyle, comfort with technology, and troubleshooting capacity.
For pen features and operating steps, see the concise walkthrough in Humalog KwikPen Guide. If you are weighing cartridge systems and refill logistics, Insulin Cartridges Guide explains device compatibility and handling. Users who need half-unit dosing or pediatric support can review format differences within pen families before choosing.
Type 2 Use and Candidates
A carefully supervised insulin pump for type 2 diabetes can be considered when multiple daily injections are complex, glucose remains variable, or dawn hyperglycemia persists. Concentrated basal insulins do not typically run in pumps; rapid-acting U-100 analogs are the standard choice. Candidates should be comfortable with carb estimation, hypoglycemia prevention, and device alarms.
People weighing advanced delivery may also revisit fundamentals in our Diabetes Articles to reinforce nutrition, activity, and sick-day routines. Those transitioning from regular human insulin can compare pharmacokinetics in Novolog vs Regular Insulin and discuss whether faster analogs align with pump features like extended boluses and temporary basal rates.
Costs, Access, and Practical Planning
Insurance coverage, formularies, and local policies can influence humalog insulin price and pump supplies. Total costs include reservoirs, infusion sets, sensors if used, and routine adhesives. Assistance programs and plan appeals may help when formulary switches occur. Always confirm the exact lispro concentration dispensed matches your device’s requirements.
Budgeting for cartridges or vials involves comparing supply cadence, discard limits, and wastage from site changes. For ways to reduce refill waste and plan inventory, see practical tips in Humalog Cartridge Savings. You can also revisit lispro use cases in Humalog Vial Rapid Insulin when deciding between vial-reservoir fills and alternate delivery paths.
Recap
Pump therapy using lispro relies on accurate programming, steady monitoring, and reliable hardware. Rapid action supports mealtime coverage and fine basal adjustments, but it also means interruptions can escalate quickly. Matching insulin action to food, activity, and illness remains core to safer daily management.
Decisions about devices, settings, and formulations benefit from individualized clinical guidance. Review labeling limits, especially concentration and compatibility, and build backup plans for set failures or power loss. With consistent technique and realistic troubleshooting steps, you can use pump therapy to support more stable glucose while minimizing day-to-day burdens.
This content is for informational purposes only and is not a substitute for professional medical advice.